If you find yourself overcome by unpleasant sensations in your legs and an irresistible urge to move them in order to relieve your discomfort you may be suffering from Restless Legs Syndrome.
What Is Restless Legs Syndrome?
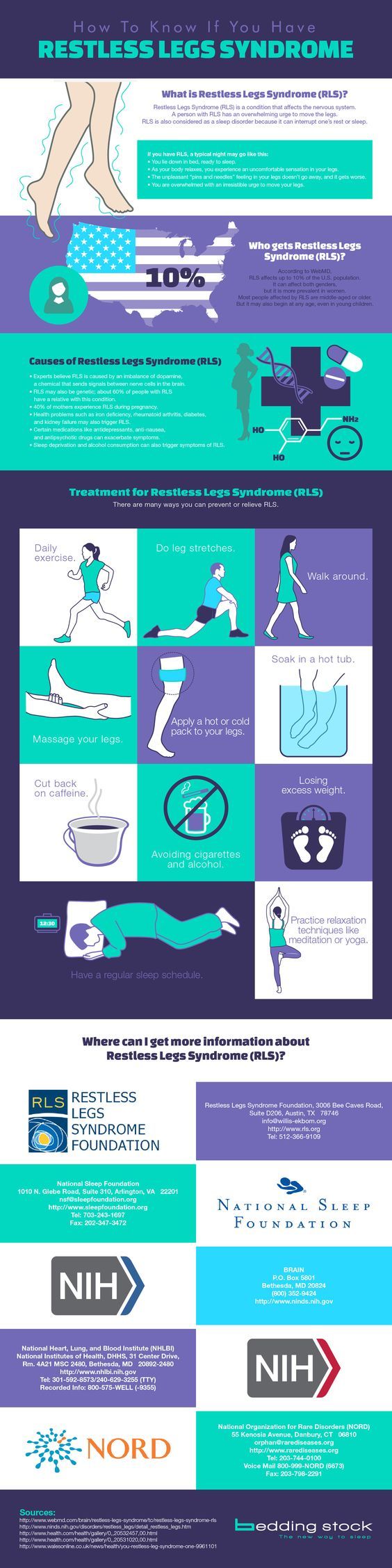
Restless Legs syndrome (RLS) is not your typical sleep disorder. Rather, it’s a neurological sensory disorder that is triggered by the act of resting, or attempting to sleep. Formally called Willis-Ekbom disease, RSL interferes with and prevents sleep by forcing sufferers to move their legs in order to relieve themselves of their symptoms.
Up to 10% of adults are affected by Restless Leg Syndrome. The disorder is slightly more common among women, and can first present itself at any age — even in very young children. However, the most severe cases are usually seen people of middle age or older.
The Symptoms of Restless Legs Syndrome (RLS)
The hallmark symptom of restless legs syndrome are uncomfortable sensations in your legs, along with an irresistible urge to move which brings relief.
People with RLS have difficulty describing the sensations they experience, but they typically use words such as: itching, throbbing, pulling, crawling or creeping. They most commonly are felt in the legs, but some people experience them in the arms and — more rarely — the chest and head. While they can affect only one side of the body, most people feel them on both sides.
In addition to the primary symptoms, over 80% of people diagnosed with RLS also have episodes of periodic limb movement of sleep (PLMS). There are twitches and jerking movements, typically of the legs but can sometimes involve the arms as well. These involuntary movements happen 2-4 times per minute, and can go on all night long.
via beddingstock.com
Symptoms of Restless Leg Syndrome Vary Widely
The symptoms of RLS can vary a lot between individuals and on a day-to-day basis. In moderate cases, people experience symptoms two or less times per week, and have a significant yet manageable disruption in their daytime functionality. Whereas in severe cases someone may be symptomatic daily, with a resulting extreme impairment in their ability to function.
Most people report that the sensations get worse in the evening, especially when their body is still, particularly if you’re sitting or lying down. While we often associate RLS with sleep, the disorder can likewise strike whenever someone is inactive for an extended period of time: such as when watching a movie, or traveling.
The severity of the sensations can also vary widely, from simply being an irritating inconvenience to bringing on extreme pain. And while moving the affected limb relieves any discomfort, the sensations typically return once you rest again.
Symptom Progression
When the disorder first develops, some people may find that their symptoms go into remission, only to reappear a few weeks or months later. However, generally symptoms get progressively worse with time.
Symptoms also progress differently depending on the cause. People who have RLS that’s caused by an underlying medical condition tend to experience a sudden onset of symptoms that increase in severity rapidly.
Whereas those who suffer from primary RLS have a much slower progression, gradually worsening over a number of years.
Quick Self-Test: Is It Restless Leg Syndrome?
If you think you may be suffering from RLS, ask yourself how many of the following statements apply to you:
- When I sit or lie down I have a strong urge to move my legs
- My desire to move is irresistible
- I’d describe these sensations as being unpleasant, creepy-crawly, itching, pulling or tugging
- Moving my legs relieves the unpleasant sensations.
- I experience most of these symptoms at night
- My jerking leg movements keep my bed partner awake at night
- I experience involuntary movements in my legs when awake
- I feel tired and have difficulty concentrating during the day
- Other members of my family experience similar symptoms
- There is no obvious physical cause of my discomfort
If you find that these describe your symptoms well, you should make an appointment with you doctor to discuss these issues.
The Impact of Restless Legs Syndrome
While restless legs syndrome is classified as a sleep disorder due to its impact on sleep, it also has more far reaching consequences for your general well-being.
Chronic sleep deprivation caused by your symptoms keeping you up at night can take a toll on your performance at work or school, and even negatively impact your social life. People suffering from RLS report having trouble concentrating, memory problems, and issues with their mood.
If left untreated, studies have shown that RLS can be responsible for a 20% decrease in daily productivity. Sleep disorders also contribute to the development of mental illnesses such as anxiety and depression.
What Causes Restless Legs Syndrome?
Restless legs syndrome can be broken down into two categories based on what is causing your symptoms: primary RLS and secondary RLS.
Secondary RLS
Secondary RLS is exactly what it sounds like: when restless legs symptoms are caused by an underlying medical condition, medication or other environmental factors.
Causes of Secondary RLS:
- Varicose veins
- Kidney disease and hemodialysisiron deficiency or anemia
- Pregnancy (Primarily in 3rd trimester)
- Peripheral neuropathy
- Alcohol, nicotine, and caffeine
- Antinausea medications
- Antipsychotics and antidepressants
- Cold and allergy medications with first generation antihistamines
Primary RLS
Primary RLS on the other hand is often referred to as idiopathic RLS because the exact cause is unknown. However, ongoing research continues to increase our understanding of the underlying mechanisms. [1]
Causes of Primary RLS
- Genes: It’s believed that these cases have a strong genetic component, and thus run in families — particularly when symptoms present before the age of 40.Numerous studies have demonstrated the link between primary RLS and a specific gene variants, and have shown that this to be responsible for about 50% of cases.RLS has likewise been linked to a gene responsible for limb development, suggesting that it may be a component of a developmental disorder.
- Dopamine Dysfunction: Evidence suggests that these genetic differences affect the activity of the neurotransmitter dopamine. Dopamine is responsible for a variety of crucial functions, but is most known for its role in signaling movement.Proper dopamine function is essential for us to be able to carry out smooth, purposeful movements. Disruption of dopamine transmission is responsible for other movement disorders, such as Parkinson’s disease. Interestingly, people with Parkinson’s have a greater likelihood of developing RLS themselves.
- Iron Deficiency: RLS has also been related to low levels of iron in the brain. Iron plays many roles in guiding the activity of brain cells, including being involved in the production of dopamine.
Whether your RLS is primary or secondary, sleep deprivation can aggravate your symptoms. Of course, when painful sensations and the irresistible urge to move take over when you lie down to rest, avoiding sleep deprivation can seem near impossible.
Practicing sleep hygiene techniques, including avoiding alcohol and caffeine; and taking naps to catch up on lost sleep can help to keep your symptoms under control.
Diagnosing Restless Legs Syndrome
Since there’s no test for restless legs syndrome, your doctor will make the diagnosis based on an assessment of your symptoms and medical history.
Your doctor will first rule out any other conditions that may be responsible for your symptoms. To do so they may order tests to check for iron deficiency, anemia, kidney failure, or pregnancy.
You’ll be asked to provide in-depth information about your symptoms and their impact on your daily functioning: How often do they occur? How long do they last? What do they feel like? How long does it take you to fall asleep?
You may be required to do a sleep study at a specialized clinic where a variety of measures will be taken while you sleep (brain waves, heartbeat, breathing, as well as leg movements). This will help your doctor rule out any other sleep disorders (such as sleep apnea), and can provide them with a better understanding of the severity of your symptoms.
The 5 Criteria for Clinical Diagnosis of RLS:
- A strong and often overwhelming need or urge to move the legs that is often associated with abnormal, unpleasant, or uncomfortable sensations.
- The urge to move the legs starts or get worse during rest or inactivity.
- The urge to move the legs is at least temporarily and partially or totally relieved by movements.
- The urge to move the legs starts or is aggravated in the evening or night.
- The above four features are not due to any other medical or behavioral condition.
Treating Restless Legs Syndrome
While there is no cure for primary restless legs syndrome, there are a variety of treatment options that can help keep your symptoms under control. Your doctor will determine treatment based on targeting your specific symptoms.
Lifestyle Changes
If your RLS is mild to moderate in severity, certain lifestyle changes can help decrease your symptoms:
- Avoid alcohol, tobacco and caffeine
- Establishing a regular sleep schedule
- Leg massages
- Hot baths, heating pads, or ice packs applied to the legs
- Aerobic exercise
- Leg stretches
- A vibrating pad called Relaxis
In 2006, a small study showed that a combination of moderate intensity aerobic exercises, along with lower-body resistance training is effective in reducing the severity of RLS symptoms by as much as 50%. Exercising just three times a week is enough to produce these results.
However, performing strenuous exercise has been demonstrated to increase RLS symptoms, so make sure you’re not pushing yourself too hard.
Yoga for Restless Legs
Some people find that performing a gentle yoga routine before bed can help reduce their symptoms and allow them to fall asleep faster. These practices are designed to increase circulation in your lower body by engaging the major muscles in your hips, back and legs; as well as encourage your nervous system to calm down through relaxation.
Medical Treatments
Medical treatments for RLS may be needed in more severe cases. However, not everyone responds to the same treatments. One drug may relieve symptoms for someone, and exacerbate them in another. Additionally, your current medication may lose effectiveness over time or even suddenly make your condition worse, requiring you to switch treatments.
You may have to go through a process of trial-and-error in order to find the treatment that works for you.
Iron Supplements
If your blood tests show that you have low iron levels, taking supplements is usually the first treatment recommended. Regular iron supplements can be purchased over-the-counter and any pharmacy. In severe cases iron will be administered via IV.
Anticonvulsants (Tegretol, Lyrica, Neurontin, and Horizant.)
Anti-seizure medications, such as gabapentin, have been successfully used to treat dopamine dysfunction in people with RLS. These medications are usually the first prescription treatment suggested, as there have been no reports of them causing symptoms to worsen; however, they do not work in all cases.
Dopamine Drugs (Mirapex, Neupro, and Requip)
RLS can also be treated with drugs typically used to treat Parkinson’s disease. These medications increase the effects of dopamine, and, when taken at night, can greatly reduce symptoms.
While these drugs are very effective, evidence has shown that over the long-term they can result in a worsening of symptoms: increasing in both frequency and severity. However, once taken off the medications people’s’ symptoms typically return to their baseline.
Narcotic Pain Relievers (Codeine, hydrocodone, or oxycodone)
If your RLS symptoms are particularly painful or if your symptoms do not respond to other medications, you may be prescribed an opiate pain reliever. These drugs can effectively control symptoms at very low doses.
Benzodiazepines (Sedatives) (Clonazepam and lorazepam)
Sedative medications are occasionally prescribed to help people with RLS sleep; they can also help to reduce muscle spasms. However, these drugs can increase daytime sleepiness, affect your ability to concentrate and are highly addictive and are thus used as a last resort treatment.
More Resources:
Restless Leg Syndrome Resources





